Unicondylar Knee Arthroplasty
Post Operative Instruction After Knee Replacement
A relatively young person with knee arthritis, which is almost exclusively on one side of the knee, with severe pain and limited ambulatory tolerance, is a candidate for uni-condylar knee replacement. When knee pain from osteoarthritis, interferes with daily activity, walking tolerance, and independence, it is time to consider this alternative. Patients may choose a uni-condylar knee replacement when they have exhausted conservative measures and they cannot maintain normal activities of daily living.
Knee Arthritis: 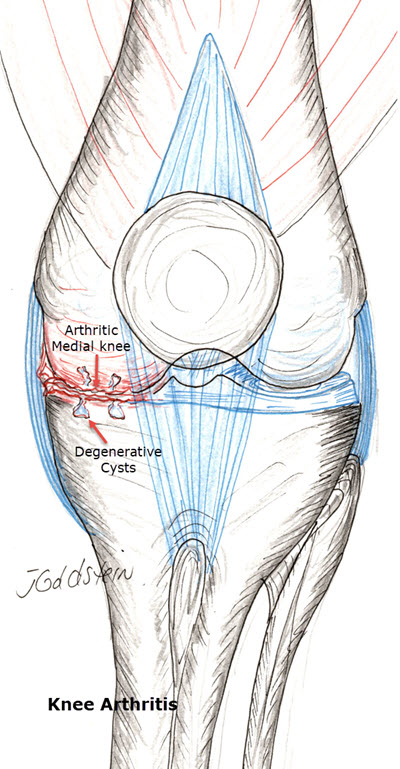
The end of the femur and tibia form the knee joint. They are covered with a thin, smooth layer of cartilage. In the knee hyaline (surface) and meniscal cartilage cushion the joint and absorb shock. Normally this cartilage is lubricated by a few drops of synovial fluid. The lining of the joint which produces this fluid is synovium. With cartilage debris from wear, the synovium proliferates and produces excess fluid. Cartilage has poor healing capabilities; as it wears away, the bone becomes exposed. The bone surfaces rubbing against each other cause pain, while cartilage has no sensation. There are no predictable or satisfactory methods for reversing the damage of arthritis when this includes a large weight-bearing area of the involved joint. When nonsurgical alternatives cannot bring a suitable level of relief, uni-condylar joint replacement is a realistic alternative. Unicondylar Knee Replacement is generally considered by Orthopedic Surgeons in patients in their 50’s unlike Total Knee Replacement, which is indicated in patients generally 60 or greater in age. This is because Total Knee Replacement at a young age is likely to fail over time, requiring revision surgery which is more complicated and maybe less successful. Revision of a Unicondylar Knee Replacement is easier and generally can be accomplished using a Primary Knee Replacement which would normally be used in an older patient initially.
Prosthetic Appearance:
A Uni-condylar Knee replacement or arthroplasty consists of three pieces. The bearing surface is made of rugged polyethylene (high-density plastic) supported by alloy metals. These components resurface the femoral and tibial surfaces on the worn side only. This has the advantage of sparing the Anterior Cruciate Ligament and Posterior Cruciate Ligament, leading to improved knee function, and usually a more normal range of motion. The femoral component (the end of the thigh bone) is made of stainless steel. The tibial component (the top of the shin bone) is a Titanium tray with the plastic insert locked in. This mates with the femoral component. There is no patellar component (kneecap) and severe patellar arthritis may be a relative contraindication to Uni-condylar Knee Replacement. Knee alignment is corrected during Unicondylar Knee Replacement to normalize loading on both sides of the knee.
Unicondylar Joint Fixation:
The components of a Unicondylar knee replacement are held to the bone with “cement”. The cement is a plastic polymer that serves as an adhesive grout.
Unicondylar Knee Replacement: 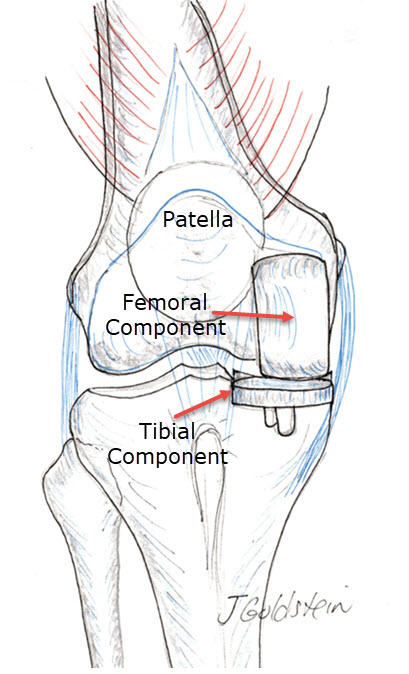
Replacement joints come in many different sizes and are precision engineered to feel and move as much like a real joint as possible. Most people with an artificial knee joint are not aware of a difference between the feel of the implant and their original knee. A Unicondylar Knee replacement allows for nearly normal motion of the knee. In the knee suitable for replacement, the range of motion is often improved following surgery. Design changes continue in existing prostheses in an effort to yield better function and longevity. A well-implanted prosthesis, in a compliant patient, usually lasts for many years. Since many prostheses now used are improved designs, we can only guess at their longevity. Trauma, wear or loosening may make it necessary to replace a uni-condylar prosthesis. Revision to a Total Knee Replacement may be necessary if the opposite side of the knee wears out. Every effort must be made to prolong the life of the Uni-condylar Knee Replacement which is implanted first. A working life of 10-15 years is reasonable, and more may be possible. Physical activity level, body weight, and patient age are strongly related to the longevity of knee replacement. The main object of a Uni-condylar Knee Replacement is relief of pain. Other goals include the correction of deformity and restoration of stability. Prosthetic design constraints limit the range of motion to approximately 0-110º. It should be emphasized that total knee replacements are not done to allow patients to return to unlimited activities and high-level sports. Fitness may be maintained by swimming, bicycling, and walking. Golfing and even skiing in some individuals may be considered, but impact loading such as running or jumping should be minimized.
![]()
Candidates for Unicondylar Knee Replacement:
The ideal patient is 50 to 60 years of age. Younger patients tend to be more active leading to premature loosening of the replacement. Young age is a relative contraindication to total knee replacement. Extreme osteoporosis (softening of the bone) or ligament instability are also relative contraindications to Unicondylar Knee replacement. In patients with a significant history of past infection of the knee, knee replacement is contraindicated because of the risk of reactivating the infection.
A patient with recurrent urinary tract infection secondary to chronic kidney stones, urethral stricture, or other genitourinary problems should have urologic evaluation prior to total knee replacement.
Precautions:
Special precautions against infection are taken before, during and after surgery. Antibiotics are used routinely peri-operatively. A special surgical room and techniques for a sterile environment are used during surgery. I always use antibiotics incorporated into the cement to lower the risk of infection. Although the risk is very low, the occurrence of late infection can be catastrophic and may require the removal of the prosthesis. To minimize the risk of infection, prophylactic antibiotics are given any time dental manipulation, urinary tract surgery or instrumentation or significant bowel procedures are performed. Any skin infection should also be treated with antibiotics as well, since late prosthetic implant infection may be related to a skin infection. There is also a risk of deep vein thrombosis (clot) after total knee replacement, and patients are generally treated with coumadin from the day before surgery until two or three weeks following surgery. This substantially reduces the risk of deep venous clot.
Hospitalization:
Patients are admitted on the day of surgery and hospitalized for one or two days. During the hospital stay, the emphasis is placed on regaining knee motion and strength, and activities of daily living. The faster patients are able to return home, the better they often do. It is unusual for Uni-condylar Knee Replacement patients to need rehabilitation before returning home. Therapy should continue at home with daily range of motion exercises, strengthening and gait training. This may be aided by the use of a home physical therapist, followed by outpatient therapy. In the highly motivated patient, therapy may be done entirely on a home program. Straight leg raising, bending over the seat of a chair, and maintaining full extension with a pillow beneath the ankle, are used with ambulation and functional exercise like an exercise bicycle to regain function.
Blood Transfusion:
Transfusion of blood is rarely necessary, especially in younger patients without a significant cardiac or pulmonary history. Blood work following surgery is monitored as a precaution.
Complications:
The most serious complication after total joint replacement is an infection. This occurs in less than 0.5% of knee replacement, but the incidence is minimized with prophylactic antibiotics and antibiotic cement. If infection occurs, removal of the prosthesis at least temporarily is often necessary. Deep venous thrombosis (clot) may also occur. This is minimized by the use of anticoagulant medication, which is started in the preoperative period and is continued for two weeks after surgery. Safe control of anticoagulation requires weekly blood tests and necessary adjustment.
Compliments of Sports Medicine and Orthopaedics, East Providence, Rhode Island
