Total Hip Replacement
Post Operative Instruction After Hip Replacement
The hip may also need replacement in some cases of fracture, although the prosthesis differs depending on patient age and bone quality as well as general health. While the baseline status of the patient and the reason for replacement are variables, Hip Replacement is nearly always successful and has an excellent outcome with the restoration of mobility and walking tolerance without pain.
Arthritis 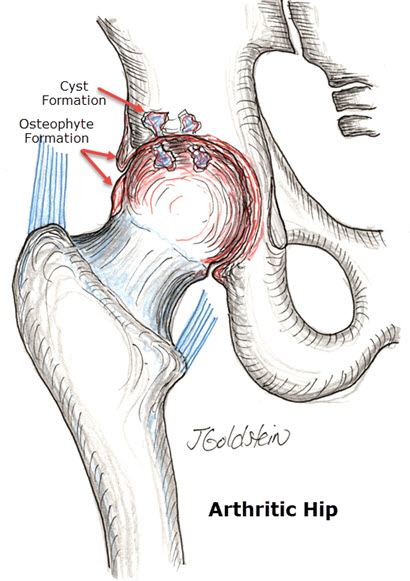
Joint surfaces are covered with a smooth layer of cartilage. This cartilage absorbs shock, and together with the normal joint lubrication provided by the joint lining, provides a smooth low friction surface. The surface cartilage has a limited capacity to heal itself. As it wears away, bone is exposed. Bone surfaces in contact cause pain while cartilage has no sensation. The inflammation caused by the debris of joint wear causes pain and stiffness, and new bone reaction leading to loss of motion.
Symptoms
Symptom onset is generally subtle. Walking tolerance usually slowly diminishes over many years to the point where only one or two blocks are possible without resting. Pain is increased by activity and cold damp weather. Anti-inflammatory medications (aspirin-related) are the mainstay of conservative treatment along with the alteration of daily activities. Swimming and bicycling are generally less painful than walking or running sports. The arthritic hip loses range of motion slowly, especially rotation.
Often the hip in need of replacement has become functionally a simple, painful hinge joint. Climbing or descending stairs or arising from a chair is especially painful. This is because the loads across the painful joint are multiplied by these activities. As a result, activities of daily living become laborious.
Diagnosis
Diagnosis is usually straightforward. Arthritis is usually easily seen on plain X-ray films, and hip motion is generally limited and painful. The pain is often in the groin or radiates into the thigh or even to the knee. Sciatica or nerve-related pain from the back may coexist, or be confused with the pain of hip arthritis. In cases where the x-ray and physical exam do not match the pain complaints, MRI, bone scan, or joint injection test may be indicated to localize the source and cause of pain.
Orthopedic Surgery
Replacement of the worn joint is usually performed on both the ball and cup except with the presence of a fracture. Generally, the cup is replaced with a metal shell which is rough on its outer surface and encourages bone ingrowth. The femoral stem is generally cemented into the marrow canal of the femoral shaft. Pressed onto this, a metal ball articulates with a hard plastic liner locked into the metal cup. This forms a stable joint and may be walked on immediately. non-cemented prostheses have been used in recent years in an attempt to increase the longevity of implants. These are only used in the active individual and more recently, most patients unless they have significant osteopenia. Early press-fit femoral stems were occasionally associated with lingering thigh discomfort. This was probably related to micro-motion of the femoral stem and has become uncommon with modern femoral stem design.
The Total Hip Replacement Candidate is ideally greater than 60 years of age and in generally good health. There should be no history of prior hip infection. In addition, any chronic or recurrent infection elsewhere may lead to late prosthetic infection. Because of this, dental abscesses should be thoroughly treated. A patient with recurrent urinary tract infection secondary to retained kidney stones, urethral strictures, or other genitourinary problems should have urology evaluation prior to total joint replacement. Antibiotics are used after surgery, during dental work, or during colonoscopy to minimize the risk of late infection. 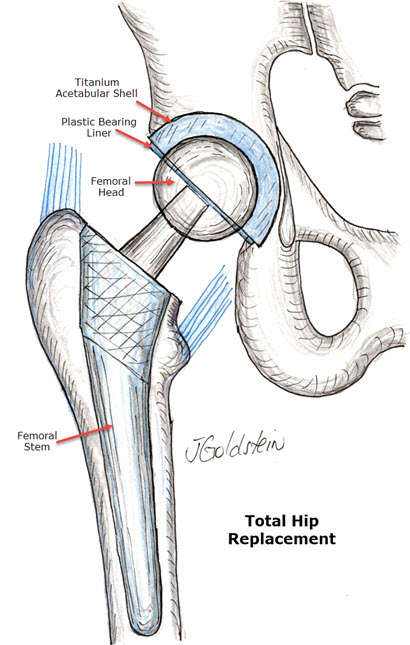
Blood Transfusion
Transfusion of blood is generally not necessary, especially in younger patients without a significant cardiac or pulmonary history. Blood work following surgery is monitored and if necessary transfusion is performed to maintain a safe blood count.
Hospitalization
Patients are admitted the day of surgery and stay generally two or three days. Depending on home support and preoperative fitness, patients may return home with home physical therapy and a home health aide or receive additional intensive physical therapy at a rehabilitation center. This decision is generally made during hospitalization when it becomes clear what functional needs will be required before discharge and depending on insurance coverage.
Complications
The most serious complication after total joint replacement is an infection. This occurs in less than 0.5% of Hip Replacements, but the incidence is minimized with prophylactic antibiotics. If infection occurs, removal of the prosthesis at least temporarily is usually necessary. Deep venous thrombosis (clot) may also occur. This is minimized by the use of anticoagulant medication, which is started in the preoperative period and is continued for two weeks after surgery. Safe control of anticoagulation requires weekly blood tests and necessary adjustment. Dislocation is extremely rare following Total Hip Replacement. This is minimized by careful prosthetic positioning and maintenance of safe hip positions for two months after surgery. Nerve injury can occur in a very small percentage of cases because of the proximity of the sciatic nerve to the hip. Leg length discrepancy may occur because of inability to restore normal length, or in occasional instances where hip stability precludes restoration of equal length. This may be normalized with a shoe lift if necessary. In nearly all instances excellent results after Total Hip Replacement allow a return to high-level function with minimal or no pain.
Compliments of Sports Medicine and Orthopaedics, East Providence, Rhode Island
